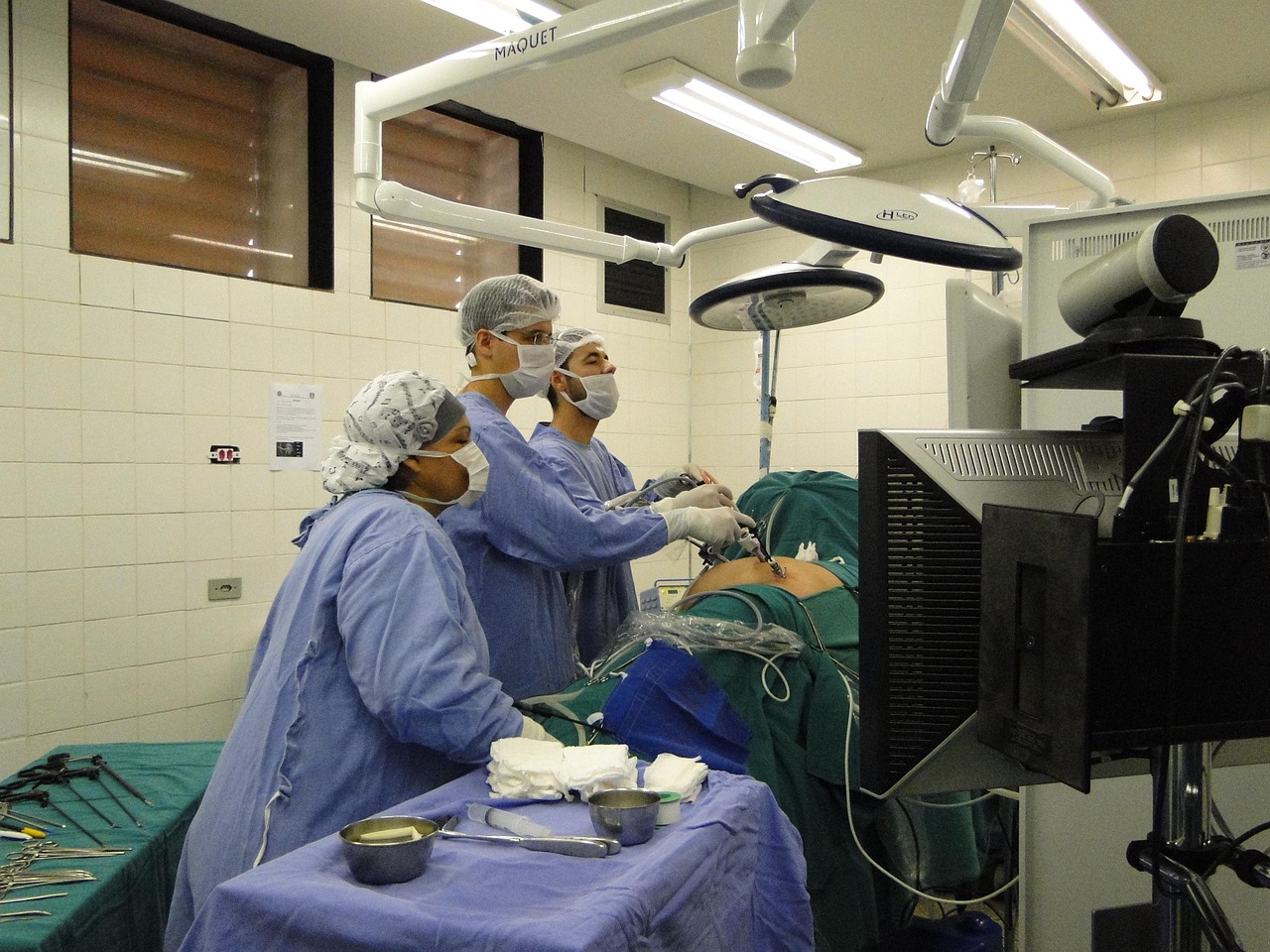
24 Mar Robotic prostatectomy explained: recovery, side effects, and nerve-sparing
A prostate cancer diagnosis raises urgent questions about timing, outcomes, and quality of life after treatment. Robotic prostatectomy is a common surgical option that removes the prostate through small incisions using robotic assistance controlled by a urologic surgeon. Patients often want to know how recovery feels day to day, how continence and erections recover over time, and whether nerve-sparing is possible.
This guide explains radical versus nerve-sparing prostatectomy in clear terms, outlines a typical hospital and catheter timeline, sets expectations for continence and erectile function recovery, and discusses realistic success and complication profiles. It also covers who may not be a candidate, when to seek a second opinion, and how Palmetto Adult and Children’s Urology coordinates pre-admission testing and insurance authorizations so logistics do not become a barrier to care.
Radical versus nerve-sparing: what is the difference?
- Radical prostatectomy refers to complete removal of the prostate and seminal vesicles for treatment of clinically localized prostate cancer. Lymph nodes may also be sampled when indicated.
- Nerve-sparing describes a surgical technique that preserves one or both neurovascular bundles that run alongside the prostate and play a key role in erections and, to a degree, early continence recovery.
Not all patients are candidates for nerve-sparing. The decision is based on cancer stage and location seen on imaging and biopsy mapping, preoperative erectile function, and the surgeon’s real-time assessment during the procedure. Cancer control is the first priority. When margins look safe, board-certified urologists at Palmetto aim to preserve nerves on one or both sides to support postoperative sexual function.
Is prostate surgery a major or minor procedure?
Prostatectomy is major surgery. Even with minimally invasive robotic assistance and small incisions, it involves removal of an internal organ, reconstruction of the urinary connection, anesthesia, and postoperative recovery with activity restrictions. Robotic techniques typically reduce blood loss and shorten hospital stays compared with open surgery, but the procedure still requires careful preparation and a structured recovery plan.
Hospital stay and catheter timeline
Most patients stay one night in the hospital after robotic prostatectomy. Some are medically ready to go home the same day or after two nights depending on pain control, nausea, mobility, and other health factors. Before discharge, you will receive catheter care instructions, walking goals, and a follow-up plan.
A urinary catheter usually remains in place for about 7 to 10 days, sometimes a little longer if healing at the bladder-urethra connection requires extra time. The catheter is removed in clinic after a quick check to confirm healing is adequate. Driving generally resumes after catheter removal once you are off prescription pain medicines and can brake comfortably; specific timing varies.
Are all robotic prostatectomies nerve-sparing?
No. Nerve-sparing is performed only when it is oncologically safe. If cancer involves or closely abuts the nerves, your surgeon may recommend partial nerve-sparing on one side or non-nerve-sparing to reduce the risk of leaving cancer behind. Preoperative erectile function, PSA trends, MRI findings, and biopsy patterns all inform this plan, which your surgeon will review with you before surgery and confirm during the operation.
Regaining bladder control after surgery
Expect some urinary leakage after catheter removal. Most patients improve steadily over weeks to months as swelling settles and pelvic floor muscles strengthen.
- Early weeks: leakage with coughing, standing, or activity is common. Using high-absorbency pads at first is reasonable; many patients downsize to thinner pads as control improves.
- First 3 months: a large portion of patients return to near-baseline daytime control by this period with continued improvement.
- By 6 to 12 months: many patients achieve good continence; a small percentage may have persistent stress incontinence that benefits from pelvic floor physical therapy or, less commonly, surgical options.
Your care team will typically recommend starting pelvic floor exercises before surgery and continuing after catheter removal. Consistent practice makes a difference.
Erectile function recovery and realistic expectations
Erection recovery depends on preoperative function, age, other health conditions, and whether one or both nerve bundles were preserved. Even with bilateral nerve-sparing, nerves can be temporarily stunned. It is common to see gradual return of erections over months. Your team may discuss rehabilitation strategies such as oral medications, vacuum erection devices, or injection therapies to encourage blood flow while nerves recover. Timelines vary; steady improvement across the first year is typical, and gains can continue beyond that.
If cancer required non-nerve-sparing surgery, spontaneous erections are less likely to return. Options still exist, including medications, vacuum devices, and penile implants. Palmetto provides comprehensive men’s sexual health support, including counseling on devices and procedures for suitable candidates.
What is the success rate of robotic prostate surgery?
Success is measured in several ways: complete cancer removal with negative margins, undetectable or very low PSA after surgery, and acceptable recovery of continence and sexual function for the individual patient. Robotic prostatectomy performed by experienced, board-certified urologists typically achieves high rates of cancer control for appropriately selected localized disease. Exact percentages depend on cancer stage, grade, preoperative PSA, and patient health. Your surgeon will review your personal risk profile and expected outcomes based on your pathology and imaging.
Who is not a candidate for robotic prostatectomy?
Surgery may not be appropriate for everyone. Situations that often steer patients and physicians toward other treatments include:
- Advanced or metastatic disease where local surgery will not provide benefit
- Significant medical conditions that make anesthesia or recovery unsafe
- Prior pelvic surgeries or anatomy that limit safe access (case by case)
- Patient preference for radiation-based therapy or active surveillance when clinically appropriate
A consultation with a urologic oncologic surgeon helps clarify options. Second opinions are always reasonable, and Palmetto supports patients in getting the information they need to decide confidently.
Complications to understand
While many patients recover without major issues, possible complications include bleeding, infection, blood clots, urinary leakage at the connection, bladder neck scarring, hernia at an incision site, and longer-term challenges with continence or erections. Your team will discuss your personal risk factors and steps taken to reduce risk, such as blood clot prevention, antibiotics when indicated, and early mobilization.
How Palmetto coordinates your care
Palmetto Adult and Children’s Urology provides a coordinated pathway from consultation to surgery and follow-up. A dedicated surgery scheduler arranges operative dates, pre-admission testing within the required window (often at least two days before surgery and up to 30 days prior when needed), and clear preoperative instructions, including fasting and guidance on aspirin or blood thinners. The team assists with prior authorization when your insurer requires it and files primary and secondary claims on your behalf. Coverage varies by plan, and patients are encouraged to verify benefits and referral requirements. For local access to prostate cancer care, you can learn more about prostate cancer treatment in North Charleston on our main site.
If you are comparing options or seeking a second opinion close to home, our providers evaluate patients across the Lowcountry. To explore related men’s health support after prostatectomy, such as devices and procedures for erectile function, see our page on penile implant surgery in Summerville for context on one of several restorative options.
FAQ
- Is prostate surgery major or minor? It is major surgery, even with minimally invasive robotic techniques.
- How long is the hospital stay? Most patients stay one night; some go home the same day or need a second night based on recovery needs.
- Are all procedures nerve-sparing? No. Nerve-sparing is performed only when cancer location and safety allow.
- How long to regain bladder control? Leakage is common at first. Many patients improve notably over the first 3 months, with continued gains by 6 to 12 months, especially with pelvic floor exercises.
- What is the success rate? High cancer control rates are typical for localized disease treated by experienced surgeons, but results depend on stage, grade, PSA, and individual health.
- Who is not a candidate? Patients with metastatic disease, high surgical risk from medical conditions, or anatomy that precludes safe access may be better served with other treatments. Preferences for radiation or surveillance, when appropriate, also guide decisions.
Next steps
If you are considering robotic prostatectomy or weighing surgery against radiation or surveillance, schedule a consultation to review your pathology, PSA, imaging, and goals. Bring your medication list and questions about recovery timelines, catheter care, continence, and sexual health. Palmetto’s board-certified urologists provide clear preoperative guidance, coordinate pre-admission testing and authorizations, and support you through recovery. For regional access points and appointment information, visit our main site for Palmetto Urology in North Charleston and Summerville resources, or call (843) 797-6600, Monday through Friday, 9:00 am to 5:00 pm EST, for scheduling assistance.
